Living Well With
Peripheral Neuropathy
Neuropathy doesn't have to define your daily life. Practical strategies for foot care, fall prevention, sleep, exercise, and mental health - organized around your day from morning to night.

Daily Foot Care:
Your Most Critical Habit
For people with diabetic neuropathy especially, reduced sensation in the feet means injuries can go unnoticed for hours or days. A 5-minute morning inspection can prevent serious complications, including amputation.
-
Daily Visual Inspection Check top and bottom of both feet, between toes, and around nails. Look for cuts, blisters, redness, swelling, or discoloration. Use a mirror or ask for help if flexibility is limited.
-
Wash and Dry Thoroughly Wash with lukewarm water - never test with numb feet, always use a thermometer or elbow. Dry completely between each toe to prevent fungal infections.
-
Proper Footwear Every Time Wear well-fitted shoes with a wide toe box. Check inside shoes for objects before putting them on - a pebble you cannot feel can cause a serious wound. Never go barefoot.
-
Temperature Awareness Avoid hot surfaces, heating pads, and electric blankets near feet. Burns and frostbite can occur without pain warning signals. Wear socks to bed in cold weather.
-
Regular Podiatrist Visits See a podiatrist every 2-3 months if you have diabetic neuropathy. Do not attempt to trim corns, calluses, or ingrown toenails yourself - professional care significantly reduces complication risk.
Fall Prevention & Balance
Peripheral neuropathy is one of the leading causes of falls in older adults. Sensory loss in the feet disrupts your body's ability to detect the ground. These strategies protect your safety at home and in daily life.
Balance Exercises
Single-leg stands, heel-to-toe walking, and tai chi movements improve proprioception. Practice near a wall or chair for safety. Start with 5 minutes twice daily.
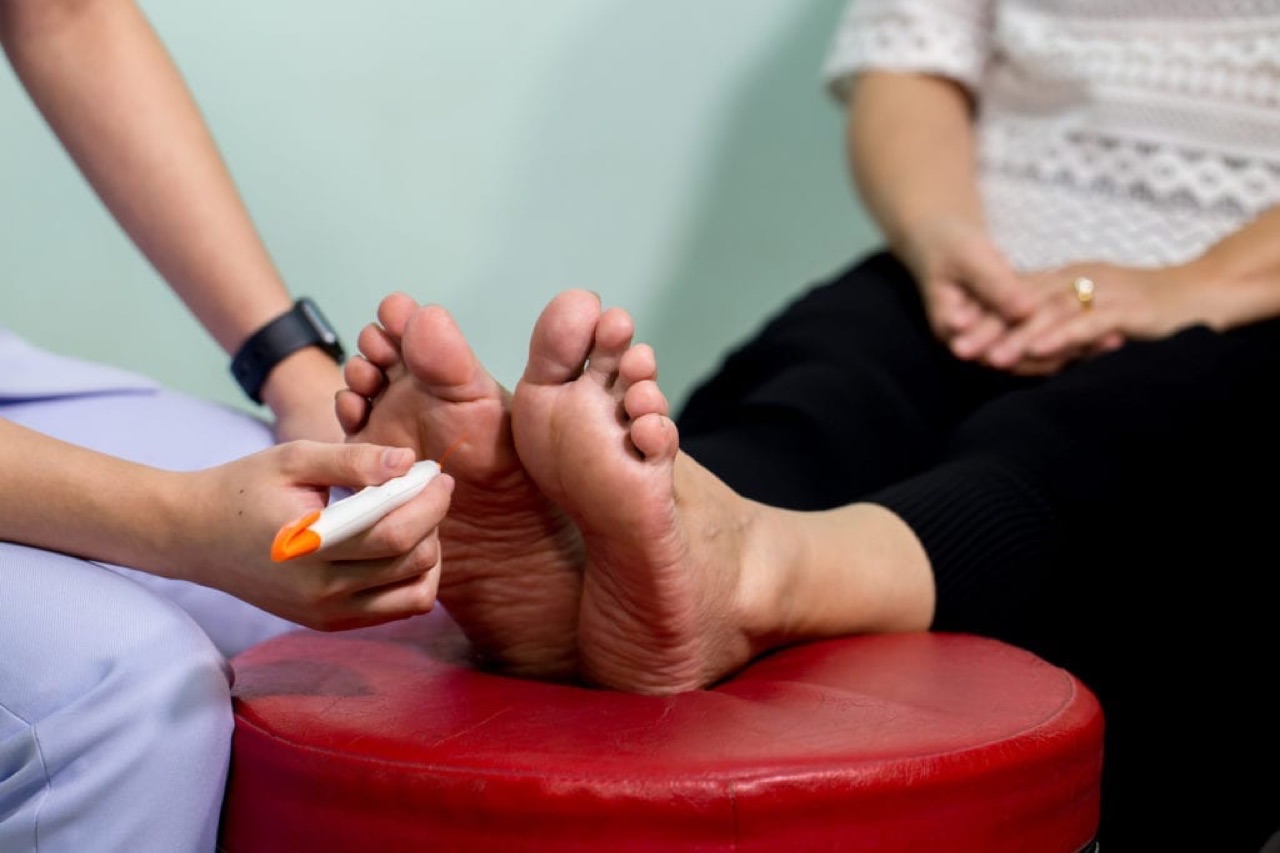
Physical Therapy
A vestibular and proprioceptive PT program tailored to neuropathy can reduce fall risk by up to 47%. Ask your neurologist for a referral.
Supportive Footwear
Compression socks (15-30 mmHg) improve circulation and provide tactile feedback. Custom orthotics can redistribute pressure and improve stability on uneven surfaces.

Exercise That Helps Nerves Heal
Regular aerobic exercise increases blood flow to peripheral nerves, promotes nerve growth factor production, and can slow neuropathy progression. The key is choosing low-impact activities that don't risk injury.
-
Walking
30 minutes of brisk walking 5 days per week improves nerve conduction velocity in multiple studies. Use supportive footwear and inspect feet afterward.
Improves nerve blood flow -
Swimming & Water Aerobics
Water supports your weight and eliminates fall risk. Warm pools (not hot) also ease burning pain symptoms and allow full range of motion without joint stress.
Zero impact, full movement -
Yoga & Stretching
Restorative yoga improves flexibility, reduces pain perception, and promotes body awareness. Gentle seated and supine poses are appropriate even for those with significant weakness.
Pain relief + body awareness -
Stationary Cycling
Recumbent bikes eliminate balance demands while providing cardiovascular benefit. Even 15 minutes daily has shown benefit in diabetic neuropathy management trials.
Safe, effective cardio
Managing Neuropathy Pain at Night
Neuropathic pain characteristically worsens at night. Reduced daytime distractions, slight drops in body temperature, and lying still all amplify nerve pain signals - making restful sleep one of the hardest challenges to solve.
Bed Cradles & Blanket Lifters
A bed cradle keeps sheets and blankets elevated off sensitive feet and legs. Even light contact from bedding triggers pain for many patients. These devices cost $30-80 and are highly effective.
Medication Timing
If you take gabapentin, pregabalin, or duloxetine, your prescriber may recommend taking the largest dose in the evening. Discuss timing adjustments - a 1-2 hour shift can significantly improve sleep quality.
Temperature Management
Cool room temperatures (65-68°F) reduce inflammatory nerve pain. Some patients find cooling gels helpful before bed; others need warmth. Trial and error with a pain diary helps identify your pattern.
TENS Before Bed
Transcutaneous electrical nerve stimulation (TENS) for 20-30 minutes before sleep activates gate control pain inhibition and often produces several hours of relief, outlasting the session itself.
Mental Health & Coping
Chronic pain rewires the brain's threat-detection system. The connection between neuropathy and depression is biological, not a character flaw - and it responds to treatment.
-
Cognitive Behavioral Therapy (CBT)
CBT for chronic pain helps reframe catastrophizing thoughts and reduces pain-related disability. Evidence from randomized trials shows CBT reduces pain interference scores even when pain intensity stays the same.
-
Support Groups
The Foundation for Peripheral Neuropathy offers in-person and virtual support groups. Peer connection reduces isolation and provides practical coping strategies not found in clinical settings.
-
Mindfulness-Based Stress Reduction
MBSR programs (8 weeks, 2.5 hrs/week) reduce pain catastrophizing and improve sleep. Multiple studies show 30-40% reductions in pain interference scores after MBSR completion.
-
Dual-Action Medications
SNRIs like duloxetine and venlafaxine treat both neuropathic pain and depression simultaneously. If your neurologist hasn't considered these, ask about them specifically.
What You Eat Affects Your Nerves
Nutritional deficiencies directly cause or worsen neuropathy. Vitamin B12 deficiency is a correctable cause of peripheral neuropathy. Alcohol is directly neurotoxic. What you eat - and avoid - matters.
Vitamin B12
Critical for myelin sheath maintenance. Deficiency is a reversible cause of neuropathy and is common in people taking metformin, PPIs, or following a vegan diet.
Alpha-Lipoic Acid
A powerful antioxidant with the strongest evidence base among supplements for diabetic neuropathy. Reduces oxidative stress in peripheral nerves.
Omega-3 Fatty Acids
EPA and DHA reduce neuroinflammation and support nerve membrane integrity. Multiple trials show improvement in nerve conduction velocity with supplementation.
B-Complex Vitamins
B1 (thiamine), B6, and folate all support nerve function. Benfotiamine (a fat-soluble form of B1) is specifically studied for diabetic neuropathy with positive results.
Vitamin D
Deficiency is strongly associated with neuropathic pain severity. Many people with chronic conditions are deficient. A simple blood test determines your level.
Antioxidant-Rich Foods
Berries, dark leafy greens, and colorful vegetables reduce systemic inflammation that worsens nerve damage. A Mediterranean-style diet pattern shows protective effects.
VA Benefits for Neuropathy
Peripheral neuropathy associated with Agent Orange exposure is a VA presumptive condition for Vietnam-era veterans, meaning you don't have to prove a direct service connection - only that you served in a qualifying location.
- Type 2 diabetes - and the neuropathy it causes - is an Agent Orange presumptive condition for qualifying veterans
- Gulf War veterans may qualify for presumptive coverage under undiagnosed illness provisions for peripheral neuropathy
- Camp Lejeune water contamination (1953-1987) has established links to neuropathic conditions
- Veterans can receive VA disability ratings of 10-80% for peripheral neuropathy affecting major extremities
- A disability rating unlocks free VA healthcare, compensation payments, and priority care access
Ready for Next Steps?
Learn about treatment options or take our symptom assessment to understand your risk level.