The signals your
nerves are sending you.
Neuropathy symptoms are the language of damaged nerves. Burning feet at night. Hands that feel like they're wearing invisible gloves. Muscles that suddenly feel unreliable. Learning what each symptom means - and how they progress - helps you communicate more effectively with your doctor and catch changes early.
Symptom Progression: Early to Advanced
Most peripheral neuropathy follows a predictable pattern - symptoms beginning distally (in the feet) and advancing proximally over months to years. The rate depends heavily on underlying cause and how quickly it's treated.
-
Sensory Changes Begin
- Intermittent tingling in toes or ball of foot
- Mild burning sensation, worse at night
- Occasional "electric shock" feelings
- Heightened sensitivity to light touch
Often dismissed as tiredness or poor circulation. Easy to overlook.
Early
OnsetWhat's Happening- Small nerve fibers being damaged first (A-delta and C fibers)
- Nerve conduction studies may still be normal
- Skin biopsy may show reduced nerve fiber density
- Blood sugar control at this stage can slow or halt progression
-
Sensory Loss & Discomfort
- Persistent numbness in feet - "stocking" distribution
- Burning pain becomes constant, especially at night
- Fingers and hands begin to be affected
- Difficulty sensing temperature in feet
- Even the weight of bedsheets causes discomfort
Moderate
StageMotor & Balance Involvement- Early muscle weakness in feet - difficulty lifting toes
- Balance problems become noticeable, especially in the dark
- Foot wounds may not be felt - infection risk rises
- Nerve conduction studies typically abnormal by now
- This is the stage where most people seek medical care
-
Significant Loss of Function
- Dense numbness from feet up to the knees
- Hands fully affected - difficulty with buttons, keys, grip
- Muscle wasting (atrophy) in lower legs visible
- Paradox: pain may decrease as fibers are destroyed
- Foot deformities (hammertoes, Charcot foot) may develop
Advanced
StageSafety & Complication Risks- Falls risk is significantly elevated - hip fractures are a major consequence
- Foot ulcers and infections are a leading cause of diabetes-related amputation
- Autonomic features (BP changes, digestive problems) often present
- Specialist-level care (neurology, podiatry) is essential
- Physical therapy critical to preserve mobility and prevent falls
Sensory Symptoms
Sensory symptoms are the most common reason people seek care for neuropathy. They arise from damage to the small and large fibers that carry pain, temperature, touch, and vibration signals to the brain.
Paradoxically, neuropathy can produce both too much sensation (burning, electric pain, hypersensitivity) and too little (numbness, inability to feel a cut). Both are signs of nerve dysfunction.
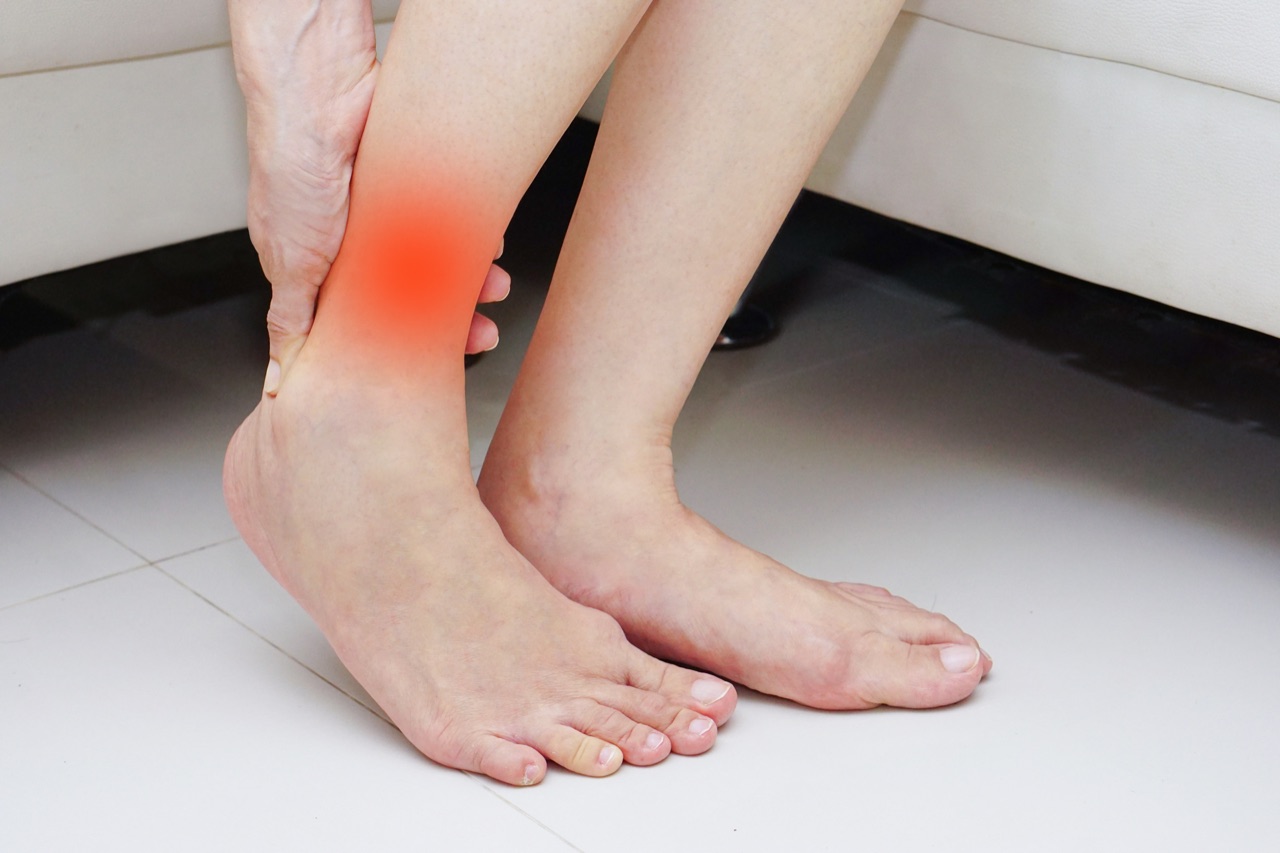
- Tingling & Pins-and-Needles
(Paresthesia) - The classic "fallen asleep" sensation - but persistent. Often the very first symptom, beginning in the toes or the balls of the feet. In small fiber neuropathy, it can be intensely unpleasant rather than merely annoying. Unlike normal positional paresthesia, neuropathic tingling persists at rest and changes character rather than resolving quickly.
- Burning Pain
- Described by patients as walking on hot coals, hot sand, or having boiling water poured over the feet. Burning neuropathy pain is typically worse at night and may be dramatically worsened by heat (a warm bed, a hot shower). It is driven by ectopic firing of damaged C fibers and responds to anticonvulsants and certain antidepressants rather than standard pain killers.
- Electric Shock Sensations
(Lancinating pain) - Brief, sudden, shooting pains like an electric current. These can be triggered by movement, touch, or occur entirely spontaneously. They are particularly common in trigeminal neuralgia, post-herpetic neuralgia (shingles-related neuropathy), and CIDP flares.
- Allodynia
- Pain from stimuli that should not be painful. The weight of a bedsheet, a light breeze across the feet, or a gentle touch causes intense discomfort. Allodynia indicates central sensitization has developed alongside the peripheral nerve damage and is a marker of more severe or prolonged neuropathy.
- Numbness & Loss of Sensation
- As nerve fibers are progressively destroyed, burning and tingling may give way to numbness. Many patients consider this a "relief" from pain, but it carries serious risks: wounds, blisters, and foreign objects in the foot go undetected, leading to infections. Loss of temperature sensation means burns from hot water bottles and heated floors are common.
- Impaired Vibration & Position Sense
(Large fiber) - Large fiber damage impairs the ability to detect vibration (tested with a 128 Hz tuning fork) and proprioception - the unconscious sense of where your limbs are in space. Standing becomes unstable, particularly with eyes closed (positive Romberg test). Walking on uneven ground, in the dark, or in a shower becomes hazardous.
Motor Symptoms
When neuropathy damages the motor fibers that carry signals from the brain to muscles, the result is weakness, impaired coordination, and - over time - muscle wasting. Motor involvement typically follows sensory symptoms but can dominate the picture in specific conditions like CIDP or Guillain-Barré.
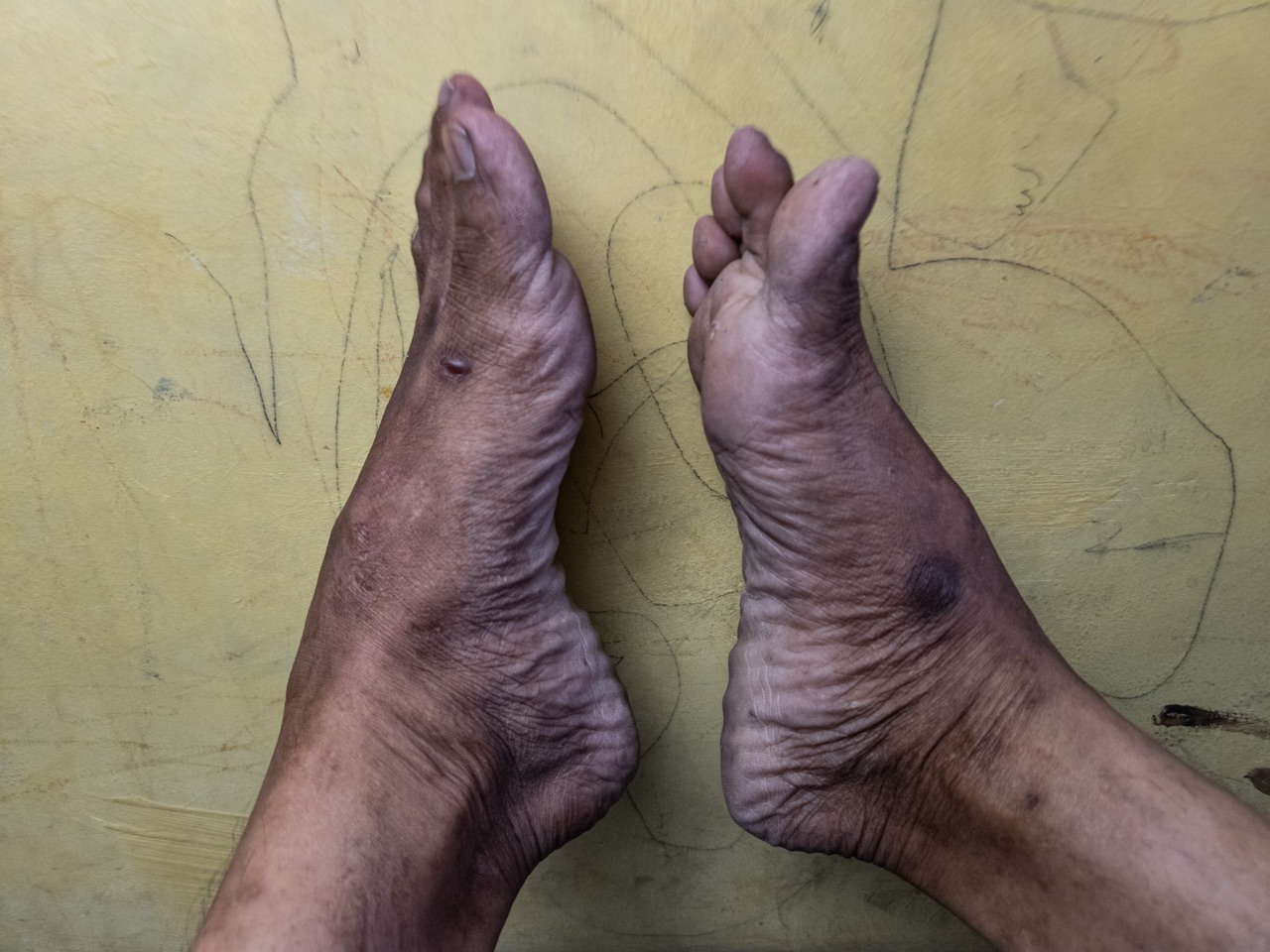
- Muscle Weakness
- Difficulty lifting the front of the foot (foot drop) is often the first motor symptom noticed - patients trip over their toes or have to lift their knees unusually high to walk. Grip strength diminishes in the hands. Climbing stairs becomes effortful as thigh muscles weaken. Any asymmetric weakness (one side significantly worse) should prompt urgent evaluation.
- Muscle Cramps & Fasciculations
- Painful involuntary muscle cramps - particularly in the calves and feet at night - are common in both diabetic and alcoholic neuropathy. Fasciculations (visible muscle twitches under the skin) indicate active nerve irritation or damage at the motor unit level. Persistent fasciculations combined with weakness warrant evaluation to rule out motor neuron disease.
- Muscle Atrophy
- In advanced neuropathy, chronically denervated muscle fibers waste away (atrophy). The intrinsic foot muscles are typically affected first, leading to a characteristic high-arched foot (pes cavus) and hammer toes - hallmarks of hereditary neuropathies like Charcot-Marie-Tooth disease. Visible wasting of the calf (peroneal atrophy) can create a distinctive "inverted champagne bottle" leg appearance.
- Balance & Gait Problems
- The combination of foot drop, proprioceptive loss, and proximal muscle weakness creates a distinctive unsteady, wide-based gait. Patients often report difficulty on stairs, escalators, and uneven surfaces. Night-time falls - particularly getting up to use the bathroom in the dark - are a major source of hip fractures in elderly neuropathy patients. Fall prevention is a key management priority.
Autonomic Symptoms
Autonomic neuropathy is the "silent" category - the nerves being damaged control internal organ functions that operate below conscious awareness. Symptoms are often attributed to other conditions for years before the neuropathic cause is recognized.
- Orthostatic Hypotension
- A sudden drop in blood pressure upon standing - typically defined as a fall of ≥20 mmHg systolic or ≥10 mmHg diastolic within 3 minutes. Causes dizziness, lightheadedness, visual dimming, and syncope (fainting). Results from failure of the autonomic reflex that normally constricts blood vessels when standing. Compression stockings, increased fluid/salt intake, and medications (midodrine, fludrocortisone) are mainstays of treatment.
- Cardiovascular Autonomic Neuropathy
- Damage to the nerves controlling heart rate leads to a fixed, elevated resting heart rate (around 90-100 bpm) with reduced heart rate variability. The normal acceleration and deceleration in response to breathing, exercise, and posture changes is blunted or absent. This is a serious complication associated with silent myocardial infarction and sudden cardiac death in diabetic patients.
- Gastroparesis & Digestive Problems
- Delayed stomach emptying causes early satiety, post-meal nausea and vomiting, bloating, and unpredictable blood sugar swings (because food absorption timing is erratic). Lower GI involvement produces alternating constipation and diarrhea - often nocturnal diarrhea, which is a nearly pathognomonic feature of diabetic autonomic neuropathy.
- Sweating Abnormalities
- Anhidrosis (inability to sweat) in the feet and lower limbs - with compensatory hyperhidrosis (excessive sweating) in the upper body and face. Anhidrosis in the feet dries and cracks the skin, creating entry points for infection. Gustatory sweating (profuse facial sweating triggered by eating) is a distinctive feature of diabetic autonomic neuropathy.
- Urogenital Symptoms
- Neurogenic bladder - impaired bladder sensation and contraction - leads to urinary retention, overflow incontinence, and recurrent urinary tract infections. In men, erectile dysfunction is often an early sign of diabetic autonomic neuropathy, frequently preceding cardiovascular autonomic involvement by several years. These symptoms are under-reported due to embarrassment but are highly treatable.
The Stocking-Glove Distribution
The most diagnostic clue in peripheral neuropathy is where symptoms occur. Because the longest nerves are most vulnerable to metabolic damage, symptoms reliably begin at the far ends of the limbs - the toes and soles of the feet - and spread proximally (toward the body) over months to years.
By the time symptoms reach the knees, the hands and fingers typically begin to be affected. This creates the characteristic distribution - as if wearing invisible stockings on the legs and gloves on the hands. The boundary of symptoms is roughly horizontal, unlike the dermatomal patterns of spinal disease.
This pattern is so characteristic that its absence - particularly unilateral symptoms, symptoms starting in the trunk, or symptoms that don't follow this distribution - should prompt investigation for a different diagnosis (radiculopathy, mononeuropathy, or an inflammatory condition).
Guillain-Barré Syndrome & Other Acute Neuropathies - Call 911
Not all neuropathy develops slowly. Guillain-Barré syndrome (GBS) is an acute, rapidly progressive immune attack on peripheral nerves that can cause paralysis within days. It is a medical emergency. Most cases begin with tingling and weakness in the feet that ascends within hours to involve the legs, torso, and arms - with the risk of life-threatening respiratory failure.
Go to the emergency room immediately if you experience any of the following, especially if symptoms are progressing rapidly over hours or days:
- Rapidly spreading weakness or paralysis
- Difficulty breathing or swallowing
- Weakness that started in the feet and is moving upward
- Sudden loss of reflexes
- Double vision or facial weakness alongside limb symptoms
- Inability to walk that developed over days, not months
- Following a recent infection (gastroenteritis, respiratory illness)
- Heart rate irregularities alongside weakness
When to See a Doctor
Many people tolerate neuropathy symptoms for months before seeking evaluation. Early intervention matters - especially in treatable causes like B12 deficiency, CIDP, or controlled diabetes. Here's a practical guide to urgency levels.
Concerning but not an emergency
- Persistent tingling or numbness in feet for more than a few weeks
- Burning foot pain that disrupts sleep
- Sensitivity to light touch on the feet
- Noticed a wound on your foot you couldn't feel
- Unsteady balance, especially in the dark
- Family history of Charcot-Marie-Tooth disease
Requires prompt evaluation
- Muscle weakness developing in legs or hands
- Foot drop - difficulty lifting the front of your foot
- Lightheadedness every time you stand up
- Symptoms spreading noticeably over weeks
- Diabetes with new neuropathy symptoms
- Suspected foot infection you couldn't feel forming
Do not wait - seek emergency care
- Weakness spreading rapidly over hours or days
- Any difficulty breathing alongside limb weakness
- Sudden facial droop or double vision
- Unable to walk - developed over days, not months
- Weakness after recent illness (GBS concern)
- Palpitations, fainting, or chest pain with neurological symptoms
Your symptoms point the way.
The pattern, timing, and location of your symptoms contain valuable diagnostic information. The next step is understanding how neuropathy is formally diagnosed - and which tests actually matter.