Peripheral Neuropathy
Peripheral neuropathy is the umbrella term for damage to the peripheral nerves - the vast network that extends from your spinal cord into your limbs, organs, and skin. It's by far the most common type, affecting over 20 million Americans.
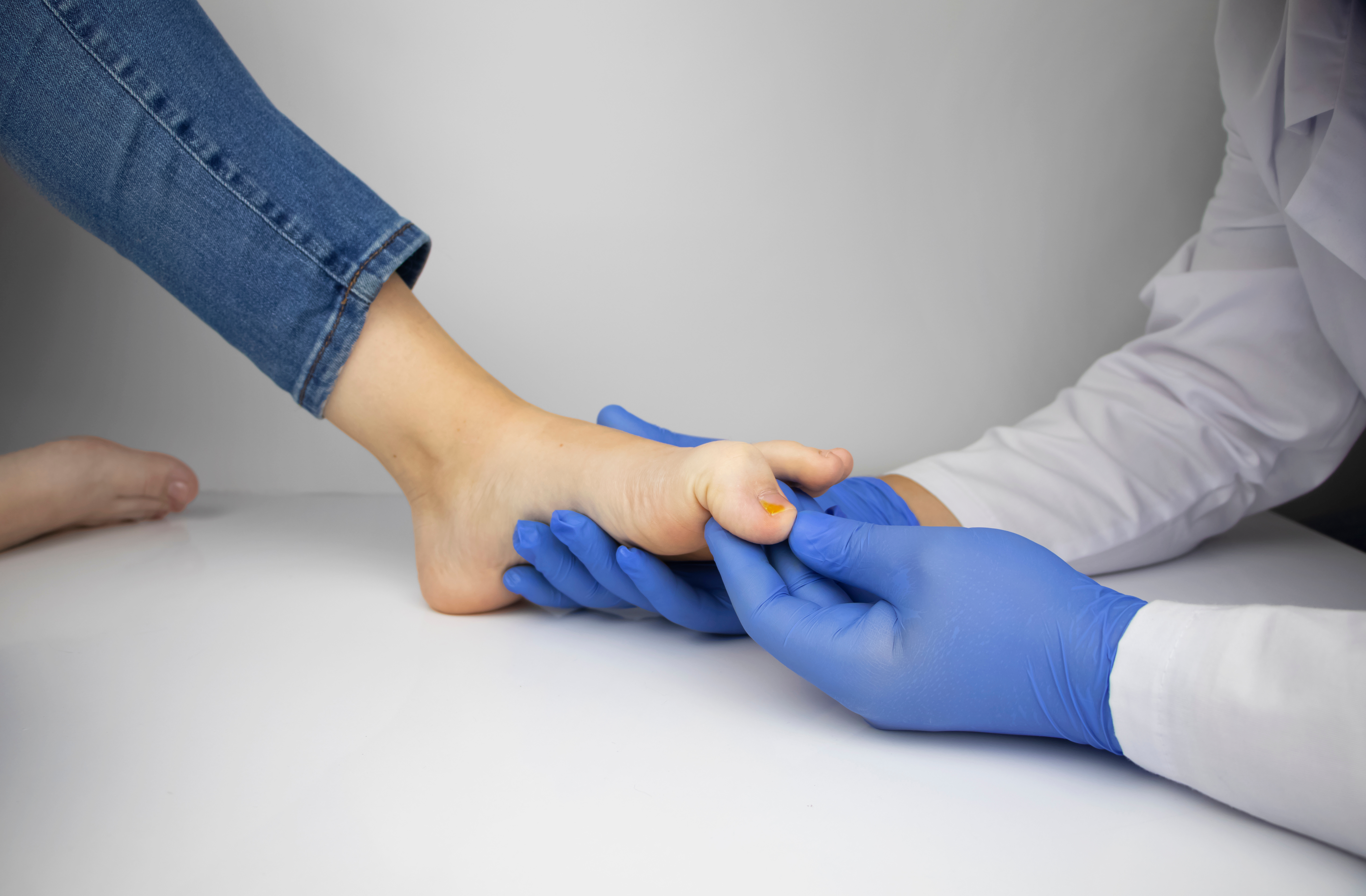
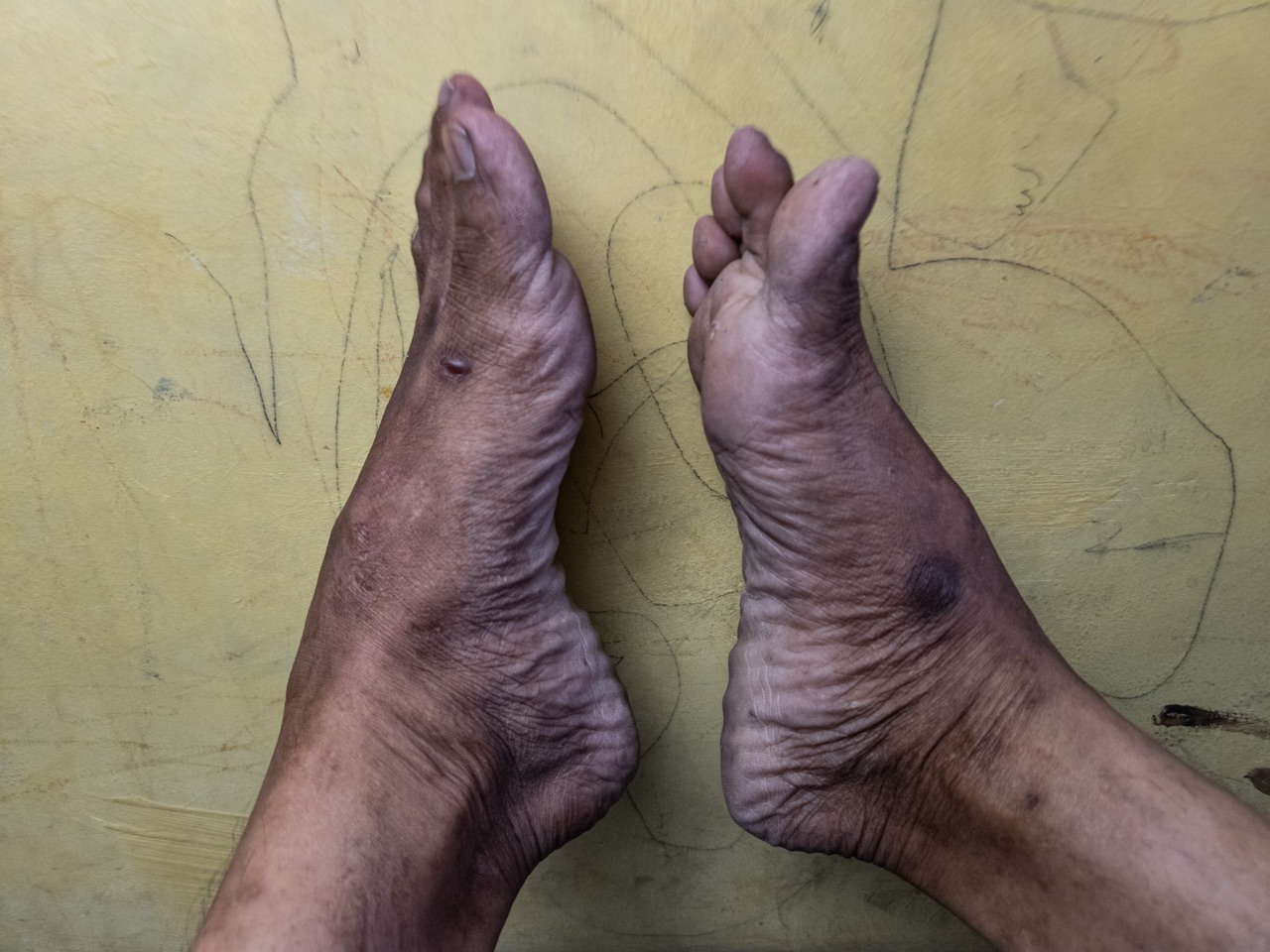
The hallmark is a length-dependent pattern: the longest nerves in the body are affected first, which is why symptoms almost always start in the feet and toes before progressing upward. This "stocking and glove" distribution is a classic diagnostic clue.
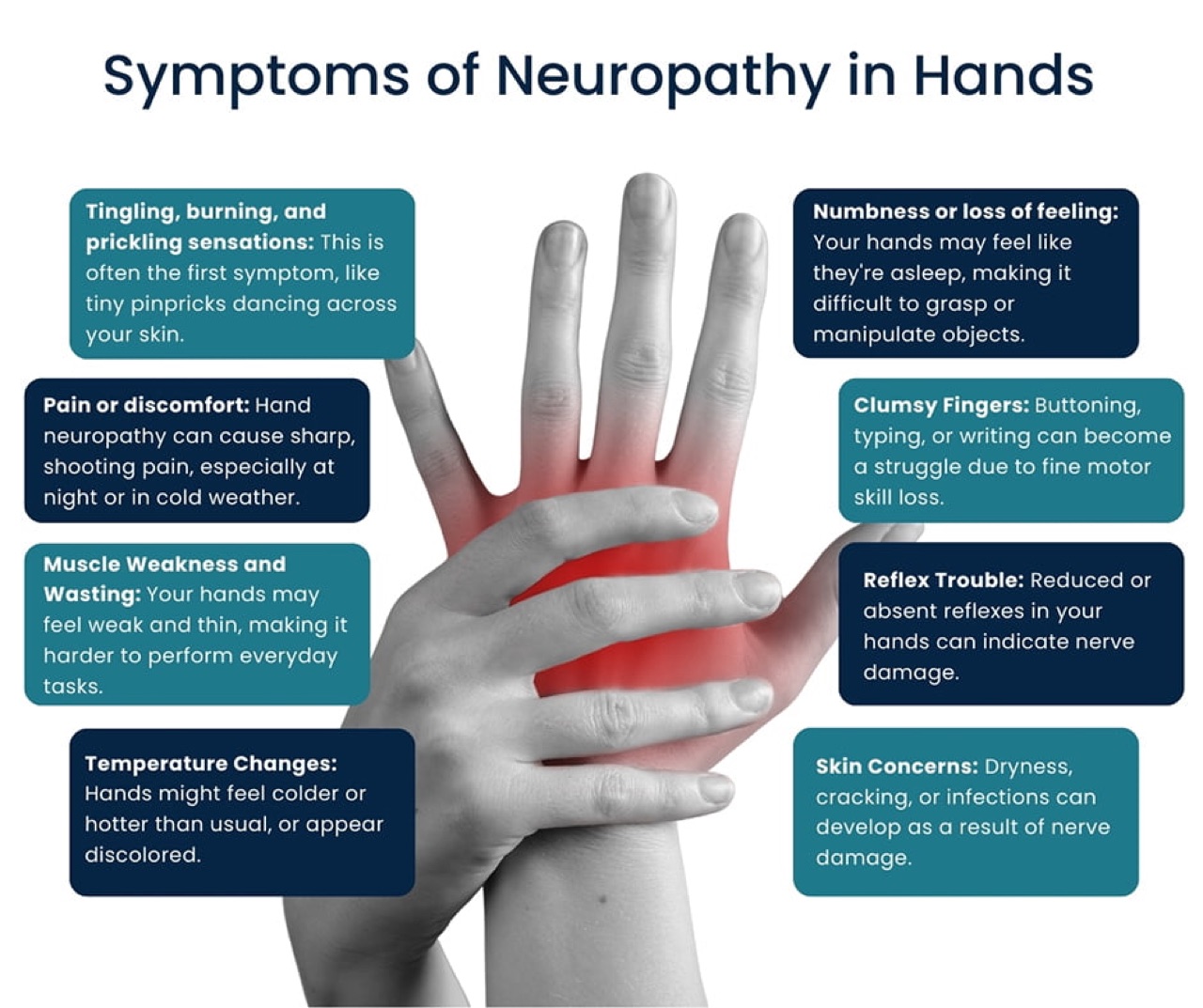
Sensory peripheral neuropathy produces tingling, burning, and numbness. Motor involvement causes muscle weakness and balance problems. Most people develop a mixed sensorimotor pattern over time.
- 50%
- of diabetics develop peripheral neuropathy
- 20M+
- Americans currently affected